User:DocElisa/sandbox
| DocElisa/Lower limbs venous ultrasonography | |
|---|---|
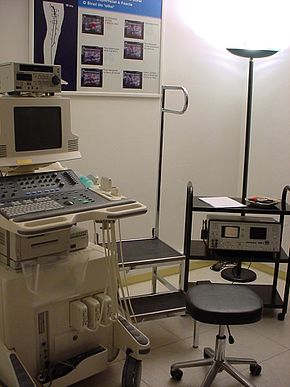 Ultrasonography equipment | |
| ICD-10-PCS | B53 |
| ICD-9-CM | 88.77 |
Ultrasonography of leg veins is a non-invasive procedure that gives information about the anatomy, physiology and pathology of both the superficial and the deep venous systems.[1]
After the introduction of ultrasound in 1956, it was very quickly adopted for use in medicine due to its rapid, accurate diagnostic capabilities which offered the possibility of prompt treatment. A few years later, acoustic Doppler velocimetry and the color doppler were devised, which have had a significant impact on many specialties, including radiology, obstetrics, gynecology, angiology and cardiology. Their use requires appropriate training in order to prevent false positive or false negative diagnoses. [2][3]
As with heart ultrasound studies, venous ultrasonography requires an understanding of hemodynamics, in order to give useful examination reports, of quality.[4] Specialized training in venous ultrasonography is not undertaken in some countries, which undermines best practice.[5]
Since lower limbs venous ultrasonography does not involve the use of radiation, the procedure is harmless and can be safely used on anybody, of any age. Preparation by the patient is not normally required. Sometimes though a complementary study of the abdominal veins is requested, in which case, the patient is asked to fast for 12 hours beforehand. The sensitivity and specificity measurements are approximately 90%. Although the equipment itself is very expensive, the actual examinations are not. This technique soon became the first choice in the diagnosis confirmation of venous pathology.[3][6]
In chronic venous insufficiency, this examination is most important in confirming the varicose disease, in allowing a proper assessment of the hemodynamics, and in enabling the charting of the disease's progression and the response to treatment. The detection of competent perforator veins may be as important as the detection of incompetent ones. Mapping[nb 1] of the venous system is essential in the understanding of the condition in any individual. This map enables vascular surgeons to plan interventions, in a stage known as virtual dissection.[nb 2][7]
......
Ultrasonography of leg veins is a non-invasive procedure that gives information about the anatomy, physiology and pathology of both the superficial and the deep venous systems.[1]
After the introduction of ultrasound in 1956, it was very quickly adopted for use in medicine due to its rapid, accurate diagnostic capabilities which offered the possibility of prompt treatment.
As with heart ultrasound studies, venous ultrasonography when performed to study venous insufficiency, varicose veins, requires an understanding of hemodynamics because the quality and the utility of the examination reports depend upon that knowledge.[4] Specialized training in venous ultrasonography is not present in some countries, which complicates best practices.[5]
This technique became the first choice to diagnosis confirmation in venous pathology, venous thrombosis and venous insufficiency. The examination protocol will be different in each of these pathologies.
Venous ultrasonography is a safe examination and can be used on people of any age. Preparation is not usually required, unless a complementary study of abdominal veins is indicated; in that case, the patient should have fasted for 12 hours. Although the equipment is costly, the examinations themselves are inexpensive.
In chronic venous insufficiency, the importance of this examination is to confirm the varicose disease, allow assessment of hemodynamics, to chart the progression of the disease over time and the response to treatment. Mapping[nb 3] of the venous system is essential to aid understanding of the condition in any individual.
Equipment
[edit]
The ultrasound equipment must be of sufficiently high quality in order to give a correct image treatment. This can then provide invaluable information, mainly at the superficial level. It must be able to deliver both doppler and color. The choice of a probe will depend on the depth needed to be studied. For example, the superficial venous system (SVS) can be very well examined using a high frequency probe of 12 MHz. For patients who have thick adipose tissue a probe of 7.5 MHz will be required. Deep veins require probes of around 6 MHz whilst the abdominal vessels are better studied with probes of between 4 and 6 MHz.[8] In summary, three probes are needed together with a top level scanner which makes it a very expensive piece of equipment. Also, the proper use of the scanner calls for a high level of expertise, so that the examiner must be well qualified and experienced in order to give effective results. In contrast to arterial ultrasonography the wall of the vein is not relevant and importance is given to the hemodynamic conclusions that the examiner can obtain in order to provide a valuable report. It follows that the examiner knowledge of venous hemodynamics is crucial, which is a real barrier to a radiologist untrained in this field, who might wish to carry out these examinations.[9][10]
Indications and contraindications
[edit]This technique became the first choice to diagnosis confirmation in venous pathology.[3][6] The sensitivity and specificity is around 90%.[6]
The purpose of this examination is focused mainly on the study of two different pathologies, venous insufficiency, and venous thrombosis.[11][12] It allows the examiner to evaluate properly:
- Superficial and deep venous network anatomy, mainly topographic anatomy.
- Blood flow direction extremely important in vein pathology.
- The presence of a retrograde blood flow (the inverse of the physiological direction, also called anterograde blood flow)[nb 4]
- The existence of a reflux situation.[13][14][nb 5]
Where venous thrombosis is suspected, this examination gives the diagnosis and evaluates the extension and the degree of severity.[15][16]
There are no contraindications for this examination. Lower limbs venous ultrasonography does not use ionizing radiation and can be used on people of any age.[17]
Mechanism
[edit]
Ultrasonography is based on the knowledge that sound can pass through human body tissues and can reflect itself on the tissue interfaces[nb 6] in the same way that light can reflect itself in a mirror. Very important for its propagation is the acoustic impedance, which means the resistance opposed by the tissue to the ultrasound pathway. No matter what tissue can reflect more or less the ultrasound beam. When two tissues have a big impedance difference, the interface between them will reflect strongly the sound. When the ultrasound beam hurts the air or a solid tissue as the bone, the difference between their impedances is so great that nearly all the acoustic energy is reflected and it will be impossible to see the underlying structures. The examiner see a shadow instead the image he would expected. This is the reason for the use of a gel between the probe and the skin. Otherwise, liquids and the blood have a low impedance, reflect few energy and they can't be visualized. There are some exceptions: when the blood flow is very slow it can be seen; is the so-called "spontaneous contrast".[18][19]
The probe is an ultrasonic sensor also called transceiver, because it performs the emission and the reception of the acoustic energy. The emission is generated on piezoelectric crystals by the so-called piezoelectric effect. The reflected ultrasound is received by the probe, transformed into an electric impulse and sent to the engine which will do the signal processing to give us the image on the screen. Depending the probe frequency, the ultrasound beam will reach a more or less depth. The higher the frequency the lesser the depth reached.[20]
Preparation
[edit]No preparation is necessary to perform this examination, except if a complementary study of abdominal veins is required, where the patient must be fasting since 12 hours.
Procedure
[edit]In a suspicion of superficial or deep thrombosis, this examination can be performed with the patient in supine position (lying down). But, if the examiner performs an evaluation for varicose veins the patient will be in standing position for a proper study of blood flow direction[21]
Deep venous thrombosis
[edit]
Unlike artery ultrasonography, the venous ultrasonography is performed with the probe in a transversal position, (perpendicular to the vessel great axis).[22] Vessels will appear on the screen as rounds, black inside. The reason for this is the fact that all collateral veins are better detected, including perforator veins, but, most important is the detection of venous thrombosis. The more reliable sign of thrombosis (even if we have a good image and color) is the absence of compressibility.[nb 7][23] If the probe is parallel to the vein axis, when the examiner compresses it, the probe can slide to the right or to the left giving a false negative for thrombosis as the vessel has disappeared. Nevertheless when the examiner needs to show in a picture the head thrombus he will present the image parallel to the vein great axis.[22]
The inability to compress the vein is one of the more reliable signs of venous thrombosis since a very recent thrombus has a low echogenicity, is seen as a black area in the gray-scale image and can be hardly visible even with very good engines. When the examiner uses color, the reliability is not better.[24] The fact that the examiner doesn't see the thrombus doesn't mean that it doesn't exist and a vein lumen with echoes doesn't mean the existence of a thrombus. The location and the thrombus detail tells us about the seriousness of the situation: in a deep venous thrombosis (DVT) or in a superficial thrombosis but with a floating thrombus, mainly if it is located near the saphenofemoral junction indicates an emergency situation as the pulmonary embolism is a high risk.[3][25]
Some teams perform a quick examination called "compression ultrasonography" in emergency situations and at bedside. It is a simplified technique used for quick deep vein thrombosis diagnosis, limited to common femoral vein and popliteal vein only, instead to spend time performing the full examination. It is performed using only one test: vein compression by transducer pressure.[26]
Compression ultrasonography has both high sensitivity and specificity for detecting proximal deep vein thrombosis only in symptomatic patients. Results are not reliable when the patient is symptomless and must be checked, for example in high risk postoperative patients mainly after orthopedic surgery where there is already lower limb pain and edema secondary to surgery, thrombi are mostly localized in the calf veins and frequently are not completely occlusive.[27][28][29]
Venous insufficiency
[edit]The emphasis of an investigation for haemodynamic changes in patients with chronic venous disease is quite different from an examination for suspected deep vein thrombosis. The request for this investigation should be made by a physician who has undertaken clinical examination to provide valid reasons for investigation, a guidance as to what to look for and, if the patient's physician is a surgeon, how he pretends to treat his patient: an investigation performed to treat the patient by a stripping or laser therapy is very different from the examination performed to execute a CHIVA [nb 8] procedure for example.
Unlike the arterial ultrasound study when the examiner studies the venous insufficiency, the vein wall has not a relevant meaning but all the interest will be focused over the blood flow direction. How veins drain is the end point of this examination. On this way, venous ultrasonography became an hemodynamic examination and is reserved to examiners who have done hemodynamic studies and training and have acquired a deep knowledge about this subject.[9]
Once more, unlike the arterial ultrasound examination, blood velocity in veins has no diagnosis meaning. Veins are a draining system similar to a low pressure hydraulic system, with a laminar flow and a low velocity. This low velocity is responsible for the fact we can only detect it spontaneously with the doppler effect on the proximal and larger veins (femoral and iliac veins), where the flow is modulated by the respiratory rhythm or continuous in cases where there is a high flow. The thinner veins don't have a spontaneously flow. However, in some circumstances the blood flow is so slow that we can see some echogenic material moving within the vein.[nb 9] Is the so-called "spontaneous contrast". This image can be mistaken for a thrombus but the vein is easily compressed opposed to the thrombus non compressibility.[30]

To evidence the blood flow velocity the examiner has at his disposal some maneuvers which accelerate flow and detect valvular function:
Manual squeezing/releasing - the examiner compress the vein below the probe pushing blood in an anterograde direction. When he releases and if valves are insufficient it will appear a retrograde flow (reflux) superior to 0.5 sec.[13]
Valsalva maneuver - when the patient performs this maneuver, he augments intra-abdominal venous pressure. If the great saphenous valve at sapheno-femoral junction is insufficient, a reflux will appear.
Paraná maneuver,[nb 10] which uses a proprioceptive reflex to test venous muscle pump induced flow. A slight push to the waist, triggers a muscle contraction at leg level (to maintain posture). This maneuver is very useful to study deep veins flow and to detect valvular insufficiency, mainly at popliteal level and when there are painful or very edematous legs. [31]
Toe flexion, active foot dorsi-flexion, hyper-extension of tip toes, can also be very useful to detect perforator vein insufficiency. These maneuvers unleashes a muscle contraction and compress deep veins. If a perforator valve is insuficicnet the examiner will register a reflux flow from the deep to the superficial through the perforator vein.[32]
All these maneuvers need a more or less long training to be executed properly.
Normal blood flow is anterograde (going to the heart), and from superficial to deep veins via perforator veins. However there is two exceptions: at the sapheno-femoral junction, the GSV collaterals which drain the abdominal wall have a flow from top to bottom and can be responsible for false positive diagnosis when the examiner tests the sapheno-femoral junction. The second exception is the flow from the venous foot sole network which (around 10%) drains to the dorsal venous arch of the foot, going therefore from deep to superficial veins.[33]
Attention will be focused on blood flow direction in deep veins, superficial main veins Great saphenous vein, small saphenous vein, their collaterals, mainly the anterior accessory saphenous vein, Giacomini vein, perforator veins as well as the shunt detection[nb 11][34]
To further complicate the examination execution, in a patient with venous insufficiency, a mapping will be done, showing veins in its longitudinal aspect while the examination has been done with the probe in transversal position. This forces the physician to extrapolated quickly all images he saw in transversal to the draw he must do in longitudinal.[35][7]
 |
 |
 |
 |
Technical pitfalls
[edit]The lower limbs venous ultrasonography is one of all medical complementary examinations where the examiner knowledge and training decide the results quality.[36][37] Not only the execution is not easy but results interpretation is subjective and proportional to the examiner knowledge in venous hemodynamics. A mapping helps the reproducibility and the inter-observer agreement of this examination.[7]}[38] This situation is yet more tricky because there are dilated veins without insufficiency by hyper-debit, non dilated veins but insufficient, veins can have a discrete insufficiency in summer but they can be normal in winter and by definition, between two valves blood flows freely in both directions, anterograde and retrograde.[39] Another problem, talking about the superficial venous system, is the fact that venous anatomy is not constant, there are plenty variations (veins are where we found them, not where we look for) and in the same patient the right lower limb is not identical to the left one. The execution protocol is completely different from the artery examination and all the dynamic maneuvers need to be very well executed and are a problem for less experimented examiners. The need of a specialized training is mandatory and there is yet many countries where this presents a big problem nowadays.[40]
Particular details
[edit]Great saphenous vein
[edit]
The great saphenous vein, has its origin at the dorsal venous arch of the foot, runs up the leg and thigh medial side to reach the groin where it drains on the common femoral vein. All the way, it is located between the superficial and the deep fascia, called the saphenous compartment,[41] receives a numberless of collaterals and drains into the deep veins by perforator veins. When visualized in ultrasonography examination, this compartment with the saphenous vein looks like an eye: is the so-called "eye image".[42] This image is not exclusive to GSV. Both the Giacomini vein and the anterior accessory saphenous vein (AASV) present this "eye image", the AASV only at its proximal 1/3. All veins which are between the skin and the superficial fascia are tributaries and all veins which cross the deep fascia and join the deep venous system (SVP) are perforator veins.[12]
Three anatomic compartments can be described:
- The deep compartment or N1 (N=Network), containing the deep veins
- Saphenous compartment or N2, between the two fascia, containing saphenous veins, AASV and Giacomini
- Superficial or N3, containing a numberless tributary veins, between them one is usually seen at the medial leg, the Leonardo's vein or posterior arch vein and very often is the cause of varicose problems.
Some authors describe one more compartment N4, containing collaterals which do a bypass between two distinct points of the same vein.[43]

The compartment differentiation is very useful in ultrasonographic examination because it enables an easier systematization, the mapping execution and, if appropriate, the surgery strategic.
Being protected between two fascias, veins belonging to compartment N2 very rarely become sinuous. So, when doing the patient physical examination the clinician who detects a sinuous vein knows immediately (with a very low possibility of error) that it's not the saphenous vein but a tributary.
The sapheno-femoral junction will be tested by Valsalva maneuver and the use of color and doppler is very useful at this level.[43]
Anterior acessory saphenous vein
[edit]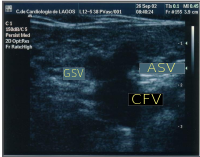
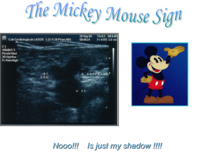
The anterior accessory saphenous vein is an important GSV collateral frequently responsible for varicose veins located on the anterior and lateral aspect of the thigh. It has a more anterior position compared with saphenous vein and is outside the femoral vessels plan. It is the "alignment sign".[12] At the groin it can be seen at the outside of great saphenous vein creating, together with the GSV and the femoral vein, an image, the so-called "Mickey mouse sign". Some authors, inspired on this sign (presented for the first time at CHIVA's meeting 2002 at Berlin), describe a "Mickey mouse view" at the groin, image formed by the common femoral vein, GSV and superficial femoral artery. When insufficient, its flow becomes retrograde and tries to drain in the superior fibular perforator, at the lateral aspect of the knee or sometimes it runs down until the ankle trying to drain in the inferior fibular perforator.[43]
Small saphenous vein
[edit]The Small saphenous vein, runs along the posterior aspect of the leg until the popliteal region where usually it drains in the popliteal vein. Ultrasonography has permitted to show a great number of variations at this level. Is not rare to see it joining the gastrocnemius vein before draining in the popliteal vein. Sometimes it doesn't contact with the popliteal vein but go up to drain in the great saphenous vein at a variable level, or, instead draining in the popliteal vein it can merge with Giacomini vein and drain in the GSV at the superior 1/3 of the thigh. Usually it connects with a perforator vein at its middle 1/3.[22] Rarely it can drain in a thigh muscle vein (semimembranosus in the images below). To check its insufficiency, Paraná maneuver is very useful.[31]
Giacomini vein
[edit]Giacomini vein acts most of the time as a bypass between GSV and SSV territories. Usually its flow is in anterograde direction, from bottom to top. However it can be retrograde without pathology. After a GSV stripping, laser ablation or after its ligation at the sapheno-femoral junction, Giacomini vein will drain into the SSV, with a retrograde flow. When there is GSV thrombosis or insufficiency, Giacomini can deviate blood flow to SSV and from this one to the popliteal vein. Each time the examiner must refer what is the flow direction in this vein, as it has important implications to decide how to treat the patient if the surgeon pretend to do a treatment other than a stripping or laser ablation.[44]
Perforator veins
[edit]
Perforator veins are a very special part of venous system, carrying blood from superficial to deep veins. During the muscular systole their valves close and don't permit the blood flow coming from the deep to the superficial veins. When their valves become insufficient they are responsible for the fast worsening of a previous varicose disease and the development of venous ulcers. The detection of competent perforator veins may be as important as the detection of incompetent ones. Detection of insufficient perforators is important because they need to be ligatured. However, the detection of competent ones is also very important because they are used strategically in new techniques of conservative surgery. When the venous ultrasonography is made, insufficient and continent perforators must be present on venous mapping.[45] To test properly these veins the examiner needs to use some maneuvers like the Paraná maneuver, toe flexion, active foot dorsi-flexion and hyper-extension of tip toes.
Examination report
[edit]
After performing this examination, the physician needs to write a report in which some points are crucial:
How is the DVS, its permeability, compressibility, continent or insufficient;
Permeability, compressibility of the SVS, presence or absence superficial insufficiency, in which veins or vein segments ;
Which perforator veins are continent or insufficient;
Presence or absence of shunts;
Mapping the insufficient veins, flux direction, shunts, perforators.[7] This map enables vascular surgeons to plan interventions, a stage known as virtual dissection.[nb 12][7]
History
[edit]Doppler effect has been described for the first time by Christian Doppler in 1843. Around forty years after the piezoelectric effect was discovered and confirmed in 1880 by Pierre & Jacques Curie, but only in the late 1940s it has been applied to the human body for medical purposes by Dr. George Ludwig, University of Pennsylvania.[46][47]
A few years later, acoustic Doppler velocimetry and the color doppler were devised, which have had a significant impact on many specialties, including radiology, obstetrics, gynecology, angiology and cardiology. Their use requires appropriate training in order to prevent false positive or false negative diagnoses. [2][3] In France, 1963, Pourcelot L. begins his these, which is presented in 1964, and used pulsed doppler for blood flow calculation [48] followed by Dr. Gene Strandness and the bio-engineering group at the University of Washington who conducted research on Doppler ultrasound as a diagnostic tool for vascular disease and published their first work in 1967, the first medical application of ultrasound.[49] [50]. The first report published about the venous system appeared around 1967-1968.[51]
Since 1970, real-time scanners and pulsed doppler, have permitted its use to study the venous system function. The first demonstration of color Doppler was achieved by Geoff Stevenson.[52][53]
After a few years, acoustic Doppler velocimetry and the color doppler were devised, which have had a significant impact on many specialties, including radiology, obstetrics, gynecology, angiology and cardiology. Its use requires appropriate training in order to prevent false positive or false negative diagnostic errors.[2][3]
Rapid technical advancements in echotomography and the possibility to see properly the superficial tissues made possible the very good specificity and sensitivity of this technique.[54] Great attention to hemodynamic study begins mainly with Franceschi, C., in France, when he described for the first time the conservative treatment for venous insufficiency in 1985.[55]
Footnotes
[edit]- ^ Mapping is the schematic design that quickly depicts the venous anatomo-functional configuration in each patient
- ^ Virtual dissection is a schema based on veins mapping where the surgeon projects what he will do to treat his patient. Drawn on paper, after the ultrasound examination, it will be drawn over the patient's skin before surgery.
- ^ Mapping is the schematic design that quickly depicts the venous anatomo-functional configuration in each patient
- ^ The anterograde blood flow or physiological blood flow in veins is from periphery to the heart
- ^ Reflux means the presence of a bi-directional flow. An isolated retrograde flow is not a reflux, but it only becomes a reflux in presence of a previously anterograde flow
- ^ Interface is the plan between two tissues with a different density, for instance skin-fat-aponevrosis-muscle
- ^ A vein can't be compressed when the blood is in a solid state (thrombus) as we cannot compress a rubber pipe if the water inside is frozen
- ^ CHIVA means "Venous Insufficiency Conservative, Hemodynamic and Ambulatory treatment" the order of words coming from French because is a procedure invented by the French researcher Claude Franceschi
- ^ Echogenic is the tissue which reflects the ultrasound beam and can be visualized on the screen
- ^ Paraná maneuver has been described for the first time by Claude Franceschi at the Chiva congress 1998 at Paraná Town, Argentina
- ^ In venous circulation, shunt is the situation where blood circulates from one vein (leak point) to another and from this one to the former (re-entry point) creating a pathway in a vicious circle between two veins one with a physiologic flow and the other with a retrograde flow
- ^ Virtual dissection is a schema based on veins mapping where the surgeon projects what he will do to treat his patient. Draw on paper, after the ultrasound examination, it will be draw over the patient's skin before surgery.
Bibliography
[edit]- Belem, Luciano Herman Juaçaba; Nogueira, Antonio Carlos Santos; Schettino, Claudio Domenico; Barros, Marcio Vinicius Lins; de Alcantara, Monica Luiza; Studart, Paulo Cesar de Carvalho; de Araújo, Paula Pimentel; do Amaral, Salomon Israel; Barretto, Simone (2004). "Normatização dos equipamentos e das técnicas para a realização de exames de ultra-sonografia vascular" [Standardization of equipment and techniques for performing vascular ultrasound examinations]. Arquivos Brasileiros de Cardiologia. 82: 1–14. doi:10.1590/S0066-782X2004001200001. PMID 15264051.
- Caggiati, A.; Ricci, S. (Dec 1997). "The long saphenous vein compartment". Phlebology. 12 (3): 107–11. doi:10.1177/026835559701200307. S2CID 70465177.
{{cite journal}}: CS1 maint: date and year (link)
- Cavezzi, A.; Labropoulos, N.; Partsch, H.; Ricci, S.; Caggiati, A.; Myers, K.; Nicolaides, A.; Smith, P.C. (2006). "Duplex Ultrasound Investigation of the Veins in Chronic Venous Disease of the Lower Limbs—UIP Consensus Document. Part II. Anatomy". European Journal of Vascular and Endovascular Surgery. 31 (3): 288–99. doi:10.1016/j.ejvs.2005.07.020. PMID 16230038.
- Cina, Alessandro; Pedicelli, Alessandro; Di Stasi, Carmine; Porcelli, Alessandra; Fiorentino, Alessandro; Cina, Gregorio; Rulli, Francesco; Bonomo, Lorenzo (2005). "Color-Doppler sonography in chronic venous insufficiency: What the radiologist should know". Current Problems in Diagnostic Radiology. 34 (2): 51–62. doi:10.1067/j.cpradiol.2004.12.001. PMID 15753879.
- Cobbold, Richard SC (2007). Foundations of Biomedical Ultrasound. New York: Oxford University Press. pp. 422–3. ISBN 978-0-19-516831-0. Retrieved February 5, 2013.
- Coleridge-Smith, P.; Labropoulos, N.; Partsch, H.; Myers, K.; Nicolaides, A.; Cavezzi, A. (2006). "Duplex Ultrasound Investigation of the Veins in Chronic Venous Disease of the Lower Limbs—UIP Consensus Document. Part I. Basic Principles". European Journal of Vascular and Endovascular Surgery. 31 (1): 83–92. doi:10.1016/j.ejvs.2005.07.019. PMID 16226898.
- Dauzat, Michel (1991). Ultrasonographie vasculaire diagnostique: Théorie et pratique [Vascular diagnostic ultrasound: Theory and practice] (in French). Paris: Vigot. pp. 386–437. ISBN 978-2-7114-1104-7.
- Elias, Antoine; Mallard, Luc; Elias, Marie; Alquier, Catherine; Guidolin, François; Gauthier, Bruno; Viard, Alain; Mahouin, Pierre; Vinel, Anne (2011). "A single complete ultrasound investigation of the venous network for the diagnostic management of patients with a clinically suspected first episode of deep venous thrombosis of the lower limbs". Thrombosis and Haemostasis. 89 (2): 221–7. doi:10.1267/THRO03020221 (inactive 2022-06-04). PMID 12574799.
{{cite journal}}: CS1 maint: DOI inactive as of June 2022 (link)
- Escribano, J.M.; Juan, J.; Bofill, R.; Rodríguez-Mori, A.; Maeso, J.; Fuentes, J.M.; Matas, M. (2005). "Haemodynamic Strategy for Treatment of Diastolic Anterograde Giacomini Varicose Veins". European Journal of Vascular and Endovascular Surgery. 30 (1): 96–101. doi:10.1016/j.ejvs.2005.03.001. PMID 15933990.
- Franceschi, Claude (1988). Théorie et Pratique de la Cure Conservatrice et Hémodynamique de l'Insuffisance Veineuse en Ambulatoire [Theory and Practice of Cure Curator and Venous hemodynamics in the outpatient clinic] (in French) (1st ed.). Précy-sous-Thil: Armançon. ISBN 2-906594-06-7.
- Markowitz, J. (1981). "Probe Selection, Machine Controls, and Equipment" (PDF). Retrieved 2013-02-24.
- Franceschi, Claude; Zamboni, Paolo (2009). Principles of Venous Hemodynamics. New York: Nova Science Publishers. ISBN 978-1-60692-485-3.
- Galeandro, Aldo Innocente; Quistelli, Giovanni; Scicchitano, Pietro; Gesualdo, Michele; Zito, Annapaola; Caputo, Paola; Carbonara, Rosa; Galgano, Giuseppe; Ciciarello, Francesco (2012). "Doppler ultrasound venous mapping of the lower limbs". Vascular Health and Risk Management. 8: 59–64. doi:10.2147/VHRM.S27552. PMC 3282606. PMID 22371652.
{{cite journal}}: CS1 maint: unflagged free DOI (link)
- Goldman, M.E., Rastegar, R. (2003). "Spontaneous echo contrast videodensity isflow-related and is dependent on the relative concentrations of fibrinogen and red blood cells". JACC. 41 (4). Retrieved 2003-02-20.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link)</ref>
- Labropoulos, Nicos; Tiongson, Jay; Pryor, Landon; Tassiopoulos, Apostolos K; Kang, Steven S; Ashraf Mansour, M; Baker, William H (2003). "Definition of venous reflux in lower-extremity veins". Journal of Vascular Surgery. 38 (4): 793–8. doi:10.1016/S0741-5214(03)00424-5. PMID 14560232. S2CID 38397552.
- Pierik, E.G.J.M.; Toonder, I.M.; van Urk, H.; Wittens, C.H.A. (1997). "Validation of duplex ultrasonography in detecting competent and incompetent perforating veins in patients with venous ulceration of the lower leg". Journal of Vascular Surgery. 26 (1): 49–52. doi:10.1016/S0741-5214(97)70146-0. PMID 9240321.
- Lam, S., Raghavendra, B.N. (1986). "Deep venous thrombosis detection by probe compression of veins". J.Ultrasound Med. 5 (2): 89–95. doi:10.7863/jum.1986.5.2.89. PMID 3514943. S2CID 25293123.
{{cite journal}}: CS1 maint: multiple names: authors list (link)
- Saliba, Orlando Adas; Giannini, Mariangela; Rollo, Hamilton Almeida (2007). "Métodos de diagnóstico não-invasivos para avaliação da insuficiência venosa dos membros inferiores" [Noninvasive diagnostic methods to evaluate venous insufficiency of the lower limbs]. Jornal Vascular Brasileiro (in Portuguese). 6 (3): 266–75. doi:10.1590/S1677-54492007000300010.
- "Lower Extremity Venous Duplex Evaluation" (PDF). Society for Vascular Ultrasound. 2011.
- Wong, J.K.F; Duncan, J.L; Nichols, D.M (2003). "Whole-leg Duplex Mapping for Varicose Veins: Observations on Patterns of Reflux in Recurrent and Primary Legs, with Clinical Correlation". European Journal of Vascular and Endovascular Surgery. 25 (3): 267–75. doi:10.1053/ejvs.2002.1830. PMID 12623340.
- Training in Diagnostic Ultrasound: Essentials, Principles and Standards: Report of a Who Study Group (PDF). Vol. 875. World Health Organization. 1998. pp. i-46, back cover. ISBN 978-92-4-120875-8. PMID 9659004. Retrieved 2013-02-05.
{{cite book}}:|journal=ignored (help)
References
[edit]- ^ a b SVU 2011.
- ^ a b c Cobbold 2003, pp. 608–609.
- ^ a b c d e f WHO 1998, pp. 1–2.
- ^ a b Franceschi & Zamboni 2009, pp. 19–28.
- ^ a b WHO 1998, pp. 7–8.
- ^ a b c Belem et al. 2004.
- ^ a b c d e Galeandro et al. 2012.
- ^ Markowitz 1981.
- ^ a b Cina et al. 2005.
- ^ Franceschi & Zamboni 2009, pp. 21–8.
- ^ WHO 1998, pp. 51–2.
- ^ a b c Cavezzi et al. 2006.
- ^ a b Labropoulos et al. 2003.
- ^ Franceschi & Zamboni 2009, p. 25.
- ^ WHO 1998, p. 26.
- ^ Dauzat 1991, pp. 386–437.
- ^ WHO 1998.
- ^ Goldman 2003.
- ^ Dauzat 1991, pp. 3–7.
- ^ Markowitz, J. "Probe Selection, Machine Controls, and Equipment" (PDF).
- ^ Franceschi 1988, p. 86.
- ^ a b c Coleridge-Smith et al. 2006.
- ^ Raghavendra 1986.
- ^ Dauzat 1991, p. 422.
- ^ Elias et al. 2011.
- ^ Hirsh J., Cogo, A. (1993). "Distribution of Thrombosis in Patients With Symptomatic Deep Vein Thrombosis Implications for simplifying the diagnosis Process with compression ultrasound". JAMA. 153 (24).
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Weir, P., Hollyoak, M. (2001). "Deep venous thrombosis in postoperative vascular surgical patients: A frequent finding without prophylaxis". JVS. 34 (4): 656–660. doi:10.1067/mva.2001.116803. PMID 11668320.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ "The Diagnostic Approach to Deep Venous Thrombosis: Diagnostic Tests for Deep Vein Thrombosis". Semin Respir Crit Care Med. 21 (6). 2000.
- ^ Lensing, A.W.A., Jongbloets, L.M.M. (May 1994). "Limitations of compression ultrasound for the detection of symptomless postoperative deep vein thrombosis". The Lancet. 343 (8906): 1142–1144. doi:10.1016/S0140-6736(94)90240-2. PMID 7910237. S2CID 23576444.
{{cite journal}}: CS1 maint: date and year (link) CS1 maint: multiple names: authors list (link) - ^ Franceschi 1988, pp. 84–5.
- ^ a b Franceschi & Zamboni 2009, p. 93.
- ^ Franceschi & Zamboni 2009, pp. 92–4.
- ^ Franceschi & Zamboni 2009, p. 19.
- ^ Franceschi & Zamboni 2009, p. 37.
- ^ Franceschi & Zamboni 2009, p. 81.
- ^ Franceschi & Zamboni 2009, pp. 9–17.
- ^ Saliba, Giannini & Rollo 2007.
- ^ Wong, Duncan & Nichols 2003.
- ^ Zamboni 2009, p. 26.
- ^ WHO 1998, p. 14.
- ^ Caggiati & Ricci 1997.
- ^ Franceschi & Zamboni 2009, p. 14.
- ^ a b c Franceschi & Zamboni 2009, pp. 11–3.
- ^ Escribano et al. 2005.
- ^ Pierik et al. 1997.
- ^ "History of the AIUM". Archived from the original on 2005-11-03. Retrieved 2013-02-24.
- ^ "The History of Ultrasound: A collection of recollections, articles, interviews and images". www.obgyn.net. Retrieved 2013-02-24.
- ^ descotes J., Pourcelot, L. (1965). "Effet Doppler et mesure du débit sanguin". C.R.Acad.Sc.Paris (261): 253–6.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ R. Eugene Zierler, MD (November 1, 2002). "D. Eugene Strandness, Jr, MD, 1928–2002". Journal of Ultrasound in Medicine.
- ^ Dauzat 1991.
- ^ Feigl P., Sigel B. (1968). "A Doppler Ultrasound method for diagnosing lower extremity venous disease". Surgery, Gynecology & Obstetrics (127): 339–350.
- ^ Baker, D.W., Eyer, M.K. (1981). "Color digital echo-doppler image presentation". Ulrasound in Med. & Bio. 7 (1): 21–31. doi:10.1016/0301-5629(81)90019-3. PMID 6165125. Retrieved 2013-02-24.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Jewell R., Persson A.V. (1989). "Use of triplex scanner in diagnosis of deep venous thrombosis". Arch. Surg. 124 (5): 593–596. doi:10.1001/archsurg.1989.01410050083017. PMID 2653279.
- ^ Dauzat M., Laroche J. P. (1983). "L'echotomographie des veines: proposition d'une méthodologie et illustration des premiers résultats pour le diagnostic des thromboses veineuse profondes". Journal d'Imagerie Médicale. 1: 193–197.
- ^ Franceschi.
___________________________________________________________________________________________________________________________________


Special:RecentChangesLinked/Wikipedia:WikiProject Medicine/Recent changes
Overview of the data model
[edit][1] The main purpose of Wikidata is to store data about things that are described by pages in Wikipedia (in any language). For example, one might want to store that the population of Berlin is 3,499,879. In this case, Berlin is the thing that is described, for example, by the article Berlin in English Wikipedia. In Wikidata, such a "thing" is represented as an Item. The Wikidata Item for Berlin would represent the thing that the Wikipedia article is about, not the Wikipedia article itself. For example, the size of Berlin is very different from the size of the Wikipedia page, and Wikidata only aims at collecting the former, not the latter.
For every Item, various pieces of information are stored in Wikidata. First, there is some basic information that clarifies what the Item is about, such as the link to a Wikipedia page in some language. There are also human readable labels and short descriptions that are used to help Wikidata users find the right Item. Second, there is a list of Statements that users have entered about the Item. Together, the information that is stored about one Item is called an ItemDescription.
Statements are the main approach of representing factual data, such as the population number in the above example. A Statement consists of two parts: a claim that something is the case (e.g., the claim "Berlin has a population of 3,499,879") and a list of references for that claim (e.g., a publication by the statistical office for Berlin-Brandenburg). The reference is given by a ReferenceRecord, and the list of references is allowed to be empty (like in Wikipedia, editors can add Statements without a reference, which might later be improved by others who know about a suitable reference).
The claim that is made in a Statement can have various forms. The most common form is a single assignment of a Value to a Property. For example, population is a Property and the number 3,499,879 is a Value. Property-Value pairs can express many different claims, and Values can be numbers, dates and times, geographic coordinates, and many more. An important special case are values that are Items. For example, one could state that Berlin is the capital of Germany, where Germany has its own Item in Wikidata, that the Property capital of refers to. Properties are defined by users, so any Property can be created. As opposed to Items, Properties do not refer to Wikipedia pages, but they do specify a Datatype for the data that they (usually) store. The data stored about Properties forms a PropertyDescription.
The individual things that Wikidata talks about, including Items and Properties, are called Entities. All Entities are Values, but many kinds of Values are not Entities (examples of the latter kind include Values for numbers, strings, and geographic coordinates). This is so since Wikidata does not intend to store Statements about individual data values, such as strings or numbers (but it could store Statements about a number as a concept that is discussed on a Wikipage, in which case the number is represented by a Wikidata Item).
Property-Value pairs are not the only kind of claims that can be given in a Statement. It is also possible to say, for example, that a Property has no Values for the given Item. For example, one can say that Angela Merkel has no children. Stating this can be relevant to distinguish it from the (common) case that the children have simply not been entered into Wikidata yet. Other things that one can say are related to classification, for example to state that Berlin is a city (i.e., "an instance of the class of all cities"). This is treated in a specific way since classification is important in many areas, e.g., in biologic taxonomies. For lack of a better name, any such basic assertion that one can make in Wikidata is called a Snak (which is small, but more than a byte). This term will not be relevant for using Wikidata (editors will not encounter it), but it is relevant for developers to avoid confusion with Statements or other claims.
For advanced usage, it is possible to make claims that consist of more than one Snak. For example, one might need to say that "the population of Berlin is 3,499,879, considering only the territory of the city, as estimated on 30 November 2011." Here, we have two additional Snaks that specify the territory the number refers to and the time when the measure was taken. It will be described below how exactly a claim can use additional Snaks.
____________________________________________________________
- Done now. If things don't work as expected, it's best to explicitly use the parameter |ref={{sfn|auth-name|year}} inside the {{cite book}} template in exactly the same style as you used in the {{sfn|auth-name|year|p=page}} template to make the references (instead of hoping that |ref=harv will work things out properly). --RexxS (talk) 22:06, 17 February 2013 (UTC)
___________________________________________________________________________
- <nowiki>
- <nowiki>
_________________________________________________________________ Medical tests
Articles about diagnostic tests or other medical tests may follow this suggested order. Many articles will only need some of these sections. This might also be a useful model for certain procedures.
While a general description of procedures may have encyclopedic value, articles about tests and other medical procedures should not provide step-by-step directions, patient instructions, disclaimers or warnings. Wikipedia is not an instruction manual and does not give medical advice.
Types, if more than one kind or variant of the test or procedure exists Indications, including contraindications Mechanism, how the test or procedure works, if it's interesting Preparation Procedure Interpretation of results, including accuracy and specificity of test results Adverse effects Legal issues, such as whether special counseling is mandated, if any History of the test
_____________________________________________________________________





