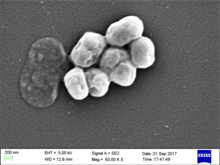
Acinetobacter baumannii
| Acinetobacter baumannii | |
|---|---|
| |
| Scientific classification | |
| Domain: | Bacteria |
| Phylum: | Pseudomonadota |
| Class: | Gammaproteobacteria |
| Order: | Pseudomonadales |
| Family: | Moraxellaceae |
| Genus: | Acinetobacter |
| Species: | A. baumannii
|
| Binomial name | |
| Acinetobacter baumannii Bouvet and Grimont 1986[1]
| |
Acinetobacter baumannii is a typically short, almost round, rod-shaped (coccobacillus) Gram-negative bacterium. It is named after the bacteriologist Paul Baumann.[2] It can be an opportunistic pathogen in humans, affecting people with compromised immune systems, and is becoming increasingly important as a hospital-derived (nosocomial) infection. While other species of the genus Acinetobacter are often found in soil samples (leading to the common misconception that A. baumannii is a soil organism, too), it is almost exclusively isolated from hospital environments.[3] Although occasionally it has been found in environmental soil and water samples,[4] its natural habitat is still not known.[citation needed]
Bacteria of this genus lack flagella but exhibit twitching or swarming motility, likely mediated by type IV pili. Motility in A. baumannii may also be due to the excretion of exopolysaccharide, creating a film of high-molecular-weight sugar chains behind the bacterium to move forward.[5] Clinical microbiologists typically differentiate members of the genus Acinetobacter from other Moraxellaceae by performing an oxidase test, as Acinetobacter spp. are the only members of the Moraxellaceae to lack cytochrome c oxidases.[6]
A. baumannii is part of the ACB complex (A. baumannii, A. calcoaceticus, and Acinetobacter genomic species 13TU). It is difficult to determine the specific species of members of the ACB complex and they comprise the most clinically relevant members of the genus.[7][8] A. baumannii has also been identified as an ESKAPE pathogen (Enterococcus faecium, Staphylococcus aureus, Klebsiella pneumoniae, Acinetobacter baumannii, Pseudomonas aeruginosa, and Enterobacter species), a group of pathogens with a high rate of antibiotic resistance that are responsible for the majority of nosocomial infections.[9]
Colloquially, A. baumannii is referred to as "Iraqibacter" due to its seemingly sudden emergence in military treatment facilities during the Iraq War.[10] It has continued to be an issue for veterans and soldiers who served in Iraq and Afghanistan. Multidrug-resistant A. baumannii has spread to civilian hospitals in part due to the transport of infected soldiers through multiple medical facilities.[5] During the COVID-19 pandemic, coinfection with A. baumannii secondary to SARS-CoV-2 infections has been reported multiple times in medical publications.[11]
OmpA
[edit]Adhesion can be a critical determinant of virulence for bacteria. The ability to attach to host cells allows bacteria to interact with them in various ways, whether by type III secretion system or simply by holding on against the prevailing movement of fluids. Outer membrane protein A (OmpA) has been shown to be involved in the adherence of A. baumannii to epithelial cells. This allows the bacteria to invade the cells through the zipper mechanism.[12] The protein was also shown to localize to the mitochondria of epithelial cells.[13] OmpA attachment to mitochondria induces it leading to swelling of mitochondria. This releases cytochrome c, which causes formation of apoptosome. This leads to the apoptosis of the cell. [14]
Antibiotic resistance
[edit]Mechanisms of antibiotic resistance can be categorized into three groups. First, resistance can be achieved by reducing membrane permeability or increasing efflux of the antibiotic and thus preventing access to the target. Second, bacteria can protect the antibiotic target through genetic mutation or post-translational modification, and last, antibiotics can be directly inactivated by hydrolysis or modification. One of the most important weapons in the armoury of Acinetobacter is its impressive genetic plasticity, facilitating rapid genetic mutations and rearrangements as well as integration of foreign determinants carried by mobile genetic elements. Of these, insertion sequences are considered one of the key forces shaping bacterial genomes and ultimately evolution.[11]
AbaR resistance islands
[edit]Pathogenicity islands, relatively common genetic structures in bacterial pathogens, are composed of two or more adjacent genes that increase a pathogen's virulence. They may contain genes that encode toxins, coagulate blood, or as in this case, allow the bacteria to resist antibiotics. AbaR-type resistance islands are typical of drug-resistant A. baumannii, and different variations may be present in a given strain. Each consists of a transposon backbone of about 16.3 Kb that facilitates horizontal gene transfer. This makes horizontal gene transfer of this and similar pathogenicity islands more likely because, when genetic material is taken up by a new bacterium, the transposons allow the pathogenicity island to integrate into the new microorganism's genome. In this case, it would grant the new microorganism the potential to resist certain antibiotics. Antibiotic resistance genes are commonly transferred between Gram-negative bacteria through plasmids via conjugation, which accelerates the appearance of new resistant strains. AbaR's contain several genes for antibiotic resistance, all flanked by insertion sequences. There exist several resistance genes circulating along A. baumannii that can be clustered in replicon groups, and may be transferred from the extensively drug-resistant Acinetobacter baumannii (XDR- AB) and New Delhi Metallo-beta-lactamase-1-producing Acinetobacter baumannii (NDM- AB) to environmental isolates of Acinetobacter spp. Conjugation experiments demonstrated that the blaOXA-23, blaPER-1, and aphA6 genes could be successfully transferred between the clinical and the environmental isolates via the plasmid group GR6 or class 1 integrons through in vitro conjugation.[15] In collaboration with some other genes, they provide resistance to aminoglycosides, aminocyclitols, tetracycline, and chloramphenicol.[16][17]
Efflux pumps
[edit]Efflux pumps are protein machines that use energy to pump antibiotics and other small molecules that get into the bacterial cytoplasm and the periplasmic space out of the cell. By constantly pumping antibiotics out of the cell, bacteria can increase the concentration of a given antibiotic required to kill them or inhibit their growth when the target of the antibiotic is inside the bacterium. A. baumannii is known to have two major efflux pumps which decrease its susceptibility to antimicrobials. The first, AdeB, has been shown to be responsible for aminoglycoside resistance.[18] The second, AdeDE, is responsible for efflux of a wide range of substrates, including tetracycline, chloramphenicol, and various carbapenems.[19] Many other efflux pumps have been implicated in A. baumannii resistant strains.[11]
Small RNA
[edit]Bacterial small RNAs are noncoding RNAs that regulate various cellular processes. Three sRNAs, AbsR11, AbsR25, and AbsR28, have been experimentally validated in the MTCC 1425 (ATCC15308) strain, which is a (multidrug-resistant) strain showing resistance to 12 antibiotics. AbsR25 sRNA could play a role in the efflux pump regulation and drug resistance.[20]
Beta-lactamase
[edit]A. baumannii has been shown to produce at least one beta-lactamase, which is an enzyme responsible for cleaving the four-atom lactam ring typical of beta-lactam antibiotics. Beta-lactam antibiotics are structurally related to penicillin, which inhibits synthesis of the bacterial cell wall. The cleaving of the lactam ring renders these antibiotics harmless to the bacteria. A. baumannii have been observed to express beta-lactamases known as Acinetobacter-derived cephalosporinases (ADCs), which are class C beta-lactamases.[21] In addition, the beta-lactamase OXA-51, a class D beta-lactamase, has been observed in A. baumannii, found to be flanked by insertion sequences, suggesting it was acquired by horizontal gene transfer.[22]
Biofilm formation
[edit]A. baumannii has been noted for its apparent ability to survive on artificial surfaces for an extended period of time, therefore allowing it to persist in the hospital environment. This is thought to be due to its ability to form biofilms.[23] For many biofilm-forming bacteria, the process is mediated by flagella. However, for A. baumannii, this process seems to be mediated by pili. Further, disruption of the putative pili chaperone and usher genes csuC and csuE were shown to inhibit biofilm formation.[24] The formation of biofilms has been shown to alter the metabolism of microorganisms within the biofilm, consequently reducing their sensitivity to antibiotics. This may be because fewer nutrients are available deeper within the biofilm. A slower metabolism can prevent the bacteria from taking up an antibiotic or performing a vital function fast enough for particular antibiotics to have an effect. They also provide a physical barrier against larger molecules and may prevent desiccation of the bacteria.[4][25] In general, biofilm formation has been linked so far with BfmRS TCS (two-component system) regulating Csu pili, Csu expression regulated by the GacSA TCS, biofilm-associated proteins BapAb, synthesis of the exopolysaccharide poly-β-1,6-N-acetylglucosamine PNAG, acyl-homoserine lactones through AbaR receptor, and AbaI autoinducer synthase. Moreover, inactivation of adeRS operon negatively affects biofilm formation and prompts decreased expression of AdeABC. Disruption of abaF has displayed an increase in fosfomycin susceptibility and a decrease in biofilm formation and virulence, suggesting a major role for this pump.[11]
The formation of biofilm involves cell attachment, a fundamental process typically triggered by environmental metabolites. A. baumannii is able to use vanillic acid as its sole carbon source, like its close relative A. baylyi. This metabolic pathway is regulated by transcriptional repressor VanR. When vanillic acid enters the cell through VanP and VanK porins it binds to the VanR regulator, which is usually bound to PvanABKP and Pcsu promoters. This binding ables the repression of PvanABKP and Pcsu promoters, which leads to increased expression of VanP and VanK porins in the cell membrane and increased expression of Csu pili. The increased expression of Csu pili results a high biofilm formation phenotype of A. baumannii. [26]
Signs and symptoms of infection
[edit]A. baumannii is an opportunistic pathogen with a range of different diseases, each with their own symptoms. Some possible types of A. baumannii infections include:[citation needed]
- Pneumonia
- Bloodstream infections
- Meningitis
- Wound and surgical site infections, including necrotizing fasciitis
- Urinary tract infections
Symptoms of A. baumannii infections are often indistinguishable from other opportunistic infections caused by other opportunistic bacteria - including Klebsiella pneumoniae and Streptococcus pneumoniae.[citation needed]
Symptoms of A. baumannii infections in turn range from fevers and chills, rash, confusion and/or altered mental states, pain or burning sensations when urinating, strong urge to urinate frequently, sensitivity to bright light, nausea (with or without vomiting), muscle and chest pains, breathing problems, and cough (with or without yellow, green, or bloody mucus).[27] In some cases, A. baumannii may present no infection or symptoms, as with colonizing an open wound or tracheostomy site.[28]
Treatment
[edit]When infections are caused by antibiotic-susceptible Acinetobacter isolates, there may be several therapeutic options, including a broad-spectrum cephalosporin (ceftazidime or cefepime), a combination beta-lactam/beta-lactamase inhibitor (i.e., one that includes sulbactam), or a carbapenem (e.g., imipenem or meropenem). Because most infections are now resistant to multiple drugs, determining what susceptibilities the particular strain has is necessary for treatment to be successful. Traditionally, infections were treated with imipenem or meropenem, but a steady rise in carbapenem-resistant A. baumannii has been noted.[29] Consequently, treatment methods often fall back on polymyxins, particularly colistin although tetracyclines have shown promise in MDR A. baumannii.[30][31] Colistin is considered a drug of last resort because it often causes kidney damage, among other side effects.[32] Prevention methods in hospitals focus on increased hand-washing and more diligent sterilization procedures.[33] An A. baumannii infection was recently treated using phage therapy.[34] Phages are viruses that attack bacteria,[35] and have also been demonstrated to resensitize A. baumannii to antibiotics it normally resists.[36]


Scientists at MIT, Harvard's Broad Institute and MIT's CSAIL found a compound named halicin using deep learning that can effectively kill A. baumannii. The compound is a repurposed drug.[37][38] The candidate drug abaucin has narrow-spectrum effectiveness.[citation needed] Zosurabalpin kills A. baumannii, is effective in animal models, and is currently in Phase I clinical trials.[39][40]
Occurrence in veterans injured in Iraq and Afghanistan
[edit]American and other western soldiers in Iraq and Afghanistan were at risk of traumatic injury due to gunfire and improvised explosive devices. Previously, infection was thought to occur due to contamination with A. baumannii at the time of injury. Subsequent studies showed that although A. baumannii may be infrequently isolated from the natural environment, the infection was more likely nosocomially acquired, likely due to the ability of A. baumannii to persist on artificial surfaces for extended periods, and the several facilities to which injured soldiers were exposed during the casualty-evacuation process. Injured soldiers were first taken to level-I facilities, where they were stabilized. Depending on the severity of the injury, the soldiers might then be transferred to a level-II facility, which consists of a forward surgical team, for additional stabilization. Depending on the logistics of the locality, the injured soldiers might be transfer between these facilities several times before finally being taken to a major hospital within the combat zone (level III). Generally after 1–3 days, when the patients were stabilized, they were transferred by air to a regional facility (level IV) for additional treatment. For soldiers serving in Iraq or Afghanistan, this was typically Landstuhl Regional Medical Center in Germany. Finally, the injured soldiers were transferred to hospitals in their home country for rehabilitation and additional treatment.[41] This repeated exposure to many different medical environments seems to be the reason A. baumannii infections have become increasingly common. Multidrug-resistant A. baumannii is a major factor in complicating the treatment and rehabilitation of injured soldiers, and has led to additional deaths.[7][42][43]
Incidence in hospitals
[edit]Being referred to as an opportunistic infection, A. baumannii infections are highly prevalent in hospital settings. A. baumannii poses very little risk to healthy individuals;[44] however, factors that increase the risks for infection include:
- Having a weakened immune system
- Chronic lung disease
- Diabetes
- Lengthened hospital stays
- Illness that requires use of a hospital ventilator
- Having an open wound treated in a hospital
- Treatments requiring invasive devices like urinary catheters
A. baumannii can be spread through direct contact with surfaces, objects, and the skin of contaminated persons.[27]
The importation of A. baumannii and subsequent presence in hospitals has been well documented.[45] A. baumannii is usually introduced into a hospital by a colonized patient. Due to its ability to survive on artificial surfaces and resist desiccation, it can remain and possibly infect new patients for some time. A baumannii growth is suspected to be favored in hospital settings due to the constant use of antibiotics by patients in the hospital.[46] Acinetobacter can be spread by person-to-person contact or contact with contaminated surfaces.[47] Acinetobacter can enter through open wounds, catheters and breathing tubes.[48] In a study of European intensive care units in 2009, A. baumannii was found to be responsible for 19.1% of ventilator-associated pneumonia cases.[49]
| Country | Reference |
|---|---|
| Australia | [50][51] |
| Brazil | [52][53][54][55] |
| China | [56][57][58][59] |
| Germany | [60][61][62] |
| India | [63][64][65] |
| South Korea | [66][67][68][69] |
| United Kingdom | [70][71] |
| United States | [72][73][74][75] |
References
[edit]- ^ Parte, A.C. "Acinetobacter". LPSN.
- ^ Lin, Ming-Feng; Lan, Chung-Yu (2014). "Antimicrobial Resistance in Acinetobacter baumannii: From Bench to Bedside". World Journal of Clinical Cases. 2 (12): 787–814. doi:10.12998/wjcc.v2.i12.787. PMC 4266826. PMID 25516853.
- ^ Antunes, Luísa C.S.; Visca, Paolo; Towner, Kevin J. (August 2014). "Acinetobacter baumannii: evolution of a global pathogen". Pathogens and Disease. 71 (3): 292–301. doi:10.1111/2049-632X.12125. PMID 24376225. S2CID 30201194.
- ^ a b Yeom, Jinki; Shin, Ji-Hyun; Yang, Ji-Young; Kim, Jungmin; Hwang, Geum-Sook; Bundy, Jacob Guy (6 March 2013). "1H NMR-Based Metabolite Profiling of Planktonic and Biofilm Cells in Acinetobacter baumannii 1656-2". PLOS ONE. 8 (3): e57730. Bibcode:2013PLoSO...857730Y. doi:10.1371/journal.pone.0057730. PMC 3590295. PMID 23483923.
- ^ a b McQueary, Christin N.; Kirkup, Benjamin C.; Si, Yuanzheng; Barlow, Miriam; Actis, Luis A.; Craft, David W.; Zurawski, Daniel V. (30 June 2012). "Extracellular stress and lipopolysaccharide modulate Acinetobacter baumannii surface-associated motility". Journal of Microbiology. 50 (3): 434–443. doi:10.1007/s12275-012-1555-1. PMID 22752907. S2CID 18294862.
- ^ Garrity, G., ed. (2000). "Pts. A & B: The Proteobacteria". Bergey's Manual of Systematic Bacteriology. Vol. 2 (2nd ed.). New York: Springer. p. 454. ISBN 978-0-387-95040-2.
- ^ a b O'Shea, MK (May 2012). "Acinetobacter in modern warfare". International Journal of Antimicrobial Agents. 39 (5): 363–75. doi:10.1016/j.ijantimicag.2012.01.018. PMID 22459899.
- ^ Gerner-Smidt, P (October 1992). "Ribotyping of the Acinetobacter calcoaceticus-Acinetobacter baumannii complex". Journal of Clinical Microbiology. 30 (10): 2680–5. doi:10.1128/JCM.30.10.2680-2685.1992. PMC 270498. PMID 1383266.
- ^ Rice, LB (15 April 2008). "Federal funding for the study of antimicrobial resistance in nosocomial pathogens: no ESKAPE". The Journal of Infectious Diseases. 197 (8): 1079–81. doi:10.1086/533452. PMID 18419525.
- ^ Drummond, Katie (2010-05-24). "Pentagon to Troop-Killing Superbugs: Resistance Is Futile". Wired.com. Condé Nast. Retrieved 8 April 2013.
- ^ a b c d Kyriakidis, I; Vasileiou, E; Pana, Z-D; Tragiannidis, A (2021). "Acinetobacter baumannii Antibiotic Resistance Mechanisms". Pathogens. 10 (373): 373. doi:10.3390/pathogens10030373. PMC 8003822. PMID 33808905.
- ^ Choi, Chul Hee; Lee, Jun Sik; Lee, Yoo Chul; Park, Tae In; Lee, Je Chul (2008). "Acinetobacter baumannii invades epithelial cells and outer membrane protein A mediates interactions with epithelial cells". BMC Microbiology. 8 (1): 216. doi:10.1186/1471-2180-8-216. PMC 2615016. PMID 19068136.
- ^ Lee, Jun Sik; Choi, Chul Hee; Kim, Jung Wook; Lee, Je Chul (23 June 2010). "Acinetobacter baumannii outer membrane protein a induces dendritic cell death through mitochondrial targeting". The Journal of Microbiology. 48 (3): 387–392. doi:10.1007/s12275-010-0155-1. PMID 20571958. S2CID 33040805.
- ^ Howard, Aoife; O’Donoghue, Michael; Feeney, Audrey; Sleator, Roy D. (May 2012). "Acinetobacter baumannii: An emerging opportunistic pathogen". Virulence. 3 (3): 243–250. doi:10.4161/viru.19700. ISSN 2150-5594. PMC 3442836. PMID 22546906.
- ^ Leungtongkam, Udomluk; Thummeepak, Rapee; Tasanapak, Kannipa; Sitthisak, Sutthirat (2018). "Acquisition and transfer of antibiotic resistance genes in association with conjugative plasmid or class 1 integrons of Acinetobacter baumannii". PLOS ONE. 13 (12): e0208468. Bibcode:2018PLoSO..1308468L. doi:10.1371/journal.pone.0208468. PMC 6283642. PMID 30521623.
- ^ Šeputienė, Vaida; Povilonis, Justas; Sužiedėlienė, Edita (April 2012). "Novel Variants of AbaR Resistance Islands with a Common Backbone in Acinetobacter baumannii Isolates of European Clone II". Antimicrobial Agents and Chemotherapy. 56 (4): 1969–1973. doi:10.1128/AAC.05678-11. PMC 3318354. PMID 22290980.
- ^ Post, V.; White, P. A.; Hall, R. M. (7 April 2010). "Evolution of AbaR-type genomic resistance islands in multiply antibiotic-resistant Acinetobacter baumannii". Journal of Antimicrobial Chemotherapy. 65 (6): 1162–1170. doi:10.1093/jac/dkq095. PMID 20375036.
- ^ Magnet, S; Courvalin, P; Lambert, T (December 2001). "Resistance-nodulation-cell division-type efflux pump involved in aminoglycoside resistance in Acinetobacter baumannii strain BM4454". Antimicrobial Agents and Chemotherapy. 45 (12): 3375–80. doi:10.1128/aac.45.12.3375-3380.2001. PMC 90840. PMID 11709311.
- ^ Chau, SL; Chu, YW; Houang, ET (October 2004). "Novel resistance-nodulation-cell division efflux system AdeDE in Acinetobacter genomic DNA group 3". Antimicrobial Agents and Chemotherapy. 48 (10): 4054–5. doi:10.1128/aac.48.10.4054-4055.2004. PMC 521926. PMID 15388479.
- ^ Sharma, Rajnikant; Arya, Sankalp; Patil, Supriya Deepak; Sharma, Atin; Jain, Pradeep Kumar; Navani, Naveen Kumar; Pathania, Ranjana (2014-01-01). "Identification of novel regulatory small RNAs in Acinetobacter baumannii". PLOS ONE. 9 (4): e93833. Bibcode:2014PLoSO...993833S. doi:10.1371/journal.pone.0093833. ISSN 1932-6203. PMC 3976366. PMID 24705412.
- ^ Périchon, Bruno; Goussard, Sylvie; Walewski, Violaine; Krizova, Lenka; Cerqueira, Gustavo; Murphy, Cheryl; Feldgarden, Michael; Wortman, Jennifer; Clermont, Dominique; Nemec, Alexandr; Courvalin, Patrice (February 2014). "Identification of 50 Class D β-Lactamases and 65 Acinetobacter-Derived Cephalosporinases in Acinetobacter spp". Antimicrobial Agents and Chemotherapy. 58 (2): 936–949. doi:10.1128/AAC.01261-13. PMC 3910822. PMID 24277043.
- ^ Higgins, PG; Pérez-Llarena, FJ; Zander, E; Fernández, A; Bou, G; Seifert, H (25 February 2013). "OXA-235, a novel Class D Beta-Lactamase Involved in Resistance to Carbapenems in Acinetobacter baumannii". Antimicrobial Agents and Chemotherapy. 57 (5): 2121–6. doi:10.1128/AAC.02413-12. PMC 3632948. PMID 23439638.
- ^ Espinal, P; Martí, S; Vila, J (January 2012). "Effect of biofilm formation on the survival of Acinetobacter baumannii on dry surfaces". The Journal of Hospital Infection. 80 (1): 56–60. doi:10.1016/j.jhin.2011.08.013. PMID 21975219.
- ^ Tomaras, AP; Dorsey, CW; Edelmann, RE; Actis, LA (December 2003). "Attachment to and biofilm formation on abiotic surfaces by Acinetobacter baumannii: involvement of a novel chaperone-usher pili assembly system". Microbiology. 149 (Pt 12): 3473–84. doi:10.1099/mic.0.26541-0. PMID 14663080.
- ^ Worthington, RJ; Richards, JJ; Melander, C (7 October 2012). "Small molecule control of bacterial biofilms". Organic & Biomolecular Chemistry. 10 (37): 7457–74. doi:10.1039/c2ob25835h. PMC 3431441. PMID 22733439.
- ^ Brychcy, Merlin; Nguyen, Brian; Tierney, Guillermo Antunez; Casula, Pranav; Kokodynski, Alexis; Godoy, Veronica G. (2024-02-03). "The metabolite vanillic acid regulates Acinetobacter baumannii surface attachment". Molecular Microbiology. doi:10.1111/mmi.15234. ISSN 0950-382X. PMID 38308563.
- ^ a b "What Is Acinetobacter Baumannii?". Everyday Health. 18 June 2015. Retrieved 18 April 2017.
- ^ "Acinetobacter". Centers for Disease Control and Prevention. 6 November 2019. Retrieved 2023-03-09.
- ^ Su, CH; Wang, JT; Hsiung, CA; Chien, LJ; et al. (2012). "Increase of carbapenem-resistant Acinetobacter baumannii infection in acute care hospitals in Taiwan: Association with hospital antimicrobial usage". PLOS One. 7 (5): e37788. Bibcode:2012PLoSO...737788S. doi:10.1371/journal.pone.0037788. PMC 3357347. PMID 22629456.
- ^ Abbo, A; Navon-Venezia, S; Hammer-Muntz, O; Krichali, T; et al. (January 2005). "Multidrug-resistant Acinetobacter baumannii". Emerging Infectious Diseases. 11 (1): 22–9. doi:10.3201/eid1101.040001. PMC 3294361. PMID 15705318.
- ^ Falagas, Matthew E.; Vardakas, Konstantinos Z.; Kapaskelis, Anastasios; Triarides, Nikolaos A.; Roussos, Nikolaos S. (May 2015). "Tetracyclines for multidrug-resistant Acinetobacter baumannii infections". International Journal of Antimicrobial Agents. 45 (5): 455–460. doi:10.1016/j.ijantimicag.2014.12.031. ISSN 1872-7913. PMID 25801348.
- ^ Spapen, H; Jacobs, R; Van Gorp, V; Troubleyn, J; et al. (25 May 2011). "Renal and neurological side effects of colistin in critically ill patients". Annals of Intensive Care. 1 (1): 14. doi:10.1186/2110-5820-1-14. PMC 3224475. PMID 21906345.
- ^ "Acinetobacter in Healthcare Settings". CDC. Retrieved 8 April 2013.
- ^ "He was dying. Antibiotics weren't working. Then doctors tried a forgotten treatment". Mother Jones. Retrieved 2018-05-17.
- ^ Altamirano, Fernando L. Gordillo; Barr, Jeremy J. (20 March 2019). "Phage Therapy in the Postantibiotic Era". Clinical Microbiology Reviews. 32 (2). doi:10.1128/CMR.00066-18. PMC 6431132. PMID 30651225.
- ^ Gordillo Altamirano, Fernando; Forsyth, John H.; Patwa, Ruzeen; Kostoulias, Xenia; Trim, Michael; Subedi, Dinesh; Archer, Stuart K.; Morris, Faye C.; Oliveira, Cody; Kielty, Luisa; Korneev, Denis; O'Bryan, Moira K.; Lithgow, Trevor J.; Peleg, Anton Y.; Barr, Jeremy J. (February 2021). "Bacteriophage-resistant Acinetobacter baumannii are resensitized to antimicrobials" (PDF). Nature Microbiology. 6 (2): 157–161. doi:10.1038/s41564-020-00830-7. PMID 33432151. S2CID 231584777.
- ^ Ray, Tiernan (13 March 2020). "MIT's deep learning found an antibiotic for a germ nothing else could kill". ZDNet.
- ^ Stokes, Jonathan M.; Yang, Kevin; Swanson, Kyle; Jin, Wengong; Cubillos-Ruiz, Andres; Donghia, Nina M.; MacNair, Craig R.; French, Shawn; Carfrae, Lindsey A.; Bloom-Ackerman, Zohar; Tran, Victoria M.; Chiappino-Pepe, Anush; Badran, Ahmed H.; Andrews, Ian W.; Chory, Emma J.; Church, George M.; Brown, Eric D.; Jaakkola, Tommi S.; Barzilay, Regina; Collins, James J. (20 February 2020). "A Deep Learning Approach to Antibiotic Discovery". Cell. 180 (4): 688–702.e13. doi:10.1016/j.cell.2020.01.021. PMC 8349178. PMID 32084340.
- ^ Zampaloni, Claudia; Mattei, Patrizio; Bleicher, Konrad; Winther, Lotte; Thäte, Claudia; Bucher, Christian; Adam, Jean-Michel; Alanine, Alexander; Amrein, Kurt E.; Baidin, Vadim; Bieniossek, Christoph; Bissantz, Caterina; Boess, Franziska; Cantrill, Carina; Clairfeuille, Thomas (January 2024). "A novel antibiotic class targeting the lipopolysaccharide transporter". Nature. 625 (7995): 566–571. Bibcode:2024Natur.625..566Z. doi:10.1038/s41586-023-06873-0. ISSN 1476-4687. PMC 10794144. PMID 38172634.
- ^ Pahil, Karanbir S.; Gilman, Morgan S. A.; Baidin, Vadim; Clairfeuille, Thomas; Mattei, Patrizio; Bieniossek, Christoph; Dey, Fabian; Muri, Dieter; Baettig, Remo; Lobritz, Michael; Bradley, Kenneth; Kruse, Andrew C.; Kahne, Daniel (January 2024). "A new antibiotic traps lipopolysaccharide in its intermembrane transporter". Nature. 625 (7995): 572–577. Bibcode:2024Natur.625..572P. doi:10.1038/s41586-023-06799-7. ISSN 1476-4687. PMC 10794137. PMID 38172635.
- ^ "Army Medical Logistics" (PDF). FM 4-02.1. United States. Archived from the original (PDF) on 2013-03-23. Retrieved April 8, 2013.
- ^ Meghoo, Colin A.; Dennis, James W.; Tuman, Caroline; Fang, Raymond (May 2012). "Diagnosis and management of evacuated casualties with cervical vascular injuries resulting from combat-related explosive blasts". Journal of Vascular Surgery. 55 (5): 1329–1337. doi:10.1016/j.jvs.2011.11.125. PMID 22325667.
- ^ Murray, Clinton K. (March 2008). "Epidemiology of Infections Associated With Combat-Related Injuries in Iraq and Afghanistan". The Journal of Trauma: Injury, Infection, and Critical Care. 64 (Supplement): S232–S238. doi:10.1097/TA.0b013e318163c3f5. PMID 18316967.
- ^ "Acinetobacter in Healthcare Settings". Centers for Disease Control and Prevention. US Department of Health and Human Services. Retrieved 18 April 2017.
- ^ Jones, Anna; Morgan, Dilys; Walsh, Amanda; Turton, Jane; Livermore, David; Pitt, Tyrone; Green, Andy; Gill, Martin; Mortiboy, Deborah (June 2006). "Importation of multidrug-resistant Acinetobacter spp infections with casualties from Iraq". The Lancet Infectious Diseases. 6 (6): 317–318. doi:10.1016/S1473-3099(06)70471-6. PMID 16728314.
- ^ Dijkshoorn, Lenie; Nemec, Alexandr; Seifert, Harald (December 2007). "An increasing threat in hospitals: multidrug-resistant Acinetobacter baumannii". Nature Reviews Microbiology. 5 (12): 939–951. doi:10.1038/nrmicro1789. PMID 18007677. S2CID 3446152.
- ^ "Acinetobacter in Healthcare Settings - HAI - CDC". www.cdc.gov. Retrieved 2 April 2018.
- ^ "Multidrug-Resistant Acinetobacter baumannii (MDRAB)." WHO Western Pacific Region, WPRO | WHO Western Pacific Region, 1 Nov. 2010, www.wpro.who.int/mediacentre/factsheets/fs_20101102/en/.
- ^ Koulenti, Despoina; Lisboa, Thiago; Brun-Buisson, Christian; Krueger, Wolfgang; Macor, Antonio; Sole-Violan, Jordi; Diaz, Emili; Topeli, Arzu; DeWaele, Jan; Carneiro, Antonio; Martin-Loeches, Ignacio; Armaganidis, Apostolos; Rello, Jordi; EU-VAP/CAP Study Group (August 2009). "Spectrum of practice in the diagnosis of nosocomial pneumonia in patients requiring mechanical ventilation in European intensive care units". Critical Care Medicine. 37 (8): 2360–2369. doi:10.1097/CCM.0b013e3181a037ac. PMID 19531951. S2CID 205537662.
- ^ Ng, J.; Gosbell, I. B.; Kelly, J. A.; Boyle, M. J.; Ferguson, J. K. (6 September 2006). "Cure of multiresistant Acinetobacter baumannii central nervous system infections with intraventricular or intrathecal colistin: case series and literature review". Journal of Antimicrobial Chemotherapy. 58 (5): 1078–1081. doi:10.1093/jac/dkl347. PMID 16916866.
- ^ Farrugia, Daniel N.; Elbourne, Liam D. H.; Hassan, Karl A.; Eijkelkamp, Bart A.; Tetu, Sasha G.; Brown, Melissa H.; Shah, Bhumika S.; Peleg, Anton Y.; Mabbutt, Bridget C.; Paulsen, Ian T.; de Crécy-Lagard, Valerie (19 March 2013). "The Complete Genome and Phenome of a Community-Acquired Acinetobacter baumannii". PLOS ONE. 8 (3): e58628. Bibcode:2013PLoSO...858628F. doi:10.1371/journal.pone.0058628. PMC 3602452. PMID 23527001.
- ^ Werneck, J. S.; Picao, R. C.; Carvalhaes, C. G.; Cardoso, J. P.; Gales, A. C. (3 December 2010). "OXA-72-producing Acinetobacter baumannii in Brazil: a case report". Journal of Antimicrobial Chemotherapy. 66 (2): 452–454. doi:10.1093/jac/dkq462. PMID 21131320.
- ^ Martins, N.; Martins, I.S.; Freitas, W.V.; Matos, J.A.; Magalhães, A.C.G.; Girão, V.B.C.; Dias, R.C.S.; Souza, T.C.; Pellegrino, F.L.P.C.; Costa, L.D.; Boasquevisque, C.H.R.; Nouér, S.A.; Riley, L.W.; Santoro-Lopes, G.; Moreira, B.M. (June 2012). "Severe infection in a lung transplant recipient caused by donor-transmitted carbapenem-resistant Acinetobacter baumannii". Transplant Infectious Disease. 14 (3): 316–320. doi:10.1111/j.1399-3062.2011.00701.x. PMC 3307813. PMID 22168176.
- ^ Superti, Silvana Vargas; Martins, Daniela de Souza; Caierão, Juliana; Soares, Fabiana da Silva; Prochnow, Taísa; Zavascki, Alexandre Prehn (April 2009). "Indications of carbapenem resistance evolution through heteroresistance as an intermediate stage in Acinetobacter baumannii after carbapenem administration". Revista do Instituto de Medicina Tropical de São Paulo. 51 (2): 111–113. doi:10.1590/s0036-46652009000200010. PMID 19390741. S2CID 21076295.
- ^ Gionco, B.; Pelayo, J. S.; Venancio, E. J.; Cayo, R.; Gales, A. C.; Carrara-Marroni, F. E. (26 June 2012). "Detection of OXA-231, a new variant of blaOXA-143, in Acinetobacter baumannii from Brazil: a case report". Journal of Antimicrobial Chemotherapy. 67 (10): 2531–2532. doi:10.1093/jac/dks223. PMID 22736746.
- ^ Zhao, W.S.; Liu, G.Y.; Mi, Z.H.; Zhang, F. (March 2011). "Coexistence of blaOXA-23 with armA and novel gyrA mutation in a pandrug-resistant Acinetobacter baumannii isolate from the blood of a patient with haematological disease in China". Journal of Hospital Infection. 77 (3): 278–279. doi:10.1016/j.jhin.2010.11.006. PMID 21281989.
- ^ Xiao, SC; Zhu, SH; Xia, ZF; Ma, B; Cheng, DS (November 2009). "Successful treatment of a critical burn patient with obstinate hyperglycemia and septic shock from pan-drug-resistant strains". Medical Science Monitor. 15 (11): CS163-5. PMID 19865060.
- ^ Wu, Yu-Chin; Hsieh, Te-Chun; Sun, Shung-Shung; Wang, Chih-Hsiu; Yen, Kuo-Yang; Lin, Yu-Yi; Kao, Chia-Hung (November 2009). "Unexpected Cloud-Like Lesion on Gallium-67 Scintigraphy: Detection of Subcutaneous Abscess Underneath the Skin With Normal Appearance in a Comatose Patient in an Intensive Care Setting". The American Journal of the Medical Sciences. 338 (5): 388. doi:10.1097/MAJ.0b013e3181a6dd36. PMID 19770790.
- ^ Duan, Xiaojun; Yang, Liu; Xia, Peiyuan (26 August 2009). "Septic arthritis of the knee caused by antibiotic-resistant Acinetobacter baumannii in a gout patient: a rare case report". Archives of Orthopaedic and Trauma Surgery. 130 (3): 381–384. doi:10.1007/s00402-009-0958-x. PMID 19707778. S2CID 37311301.
- ^ Wagner, JA; Nenoff, P; Handrick, W; Renner, R; Simon, J; Treudler, R (February 2011). "Necrotizing fasciitis caused by Acinetobacter baumannii : A case report". Der Hautarzt; Zeitschrift für Dermatologie, Venerologie, und Verwandte Gebiete (in German). 62 (2): 128–30. doi:10.1007/s00105-010-1962-3. PMID 20835812.
- ^ Aivazova, V; Kainer, F; Friese, K; Mylonas, I (January 2010). "Acinetobacter baumannii infection during pregnancy and puerperium". Archives of Gynecology and Obstetrics. 281 (1): 171–4. doi:10.1007/s00404-009-1107-z. PMID 19462176. S2CID 23112180.
- ^ Schulte, B; Goerke, C; Weyrich, P; Gröbner, S; Bahrs, C; Wolz, C; Autenrieth, IB; Borgmann, S (December 2005). "Clonal spread of meropenem-resistant Acinetobacter baumannii strains in hospitals in the Mediterranean region and transmission to South-west Germany". The Journal of Hospital Infection. 61 (4): 356–7. doi:10.1016/j.jhin.2005.05.009. PMID 16213625.
- ^ Piparsania, S; Rajput, N; Bhatambare, G (September–October 2012). "Intraventricular polymyxin B for the treatment of neonatal meningo-ventriculitis caused by multi-resistant Acinetobacter baumannii--case report and review of literature". The Turkish Journal of Pediatrics. 54 (5): 548–54. PMID 23427525.
- ^ John, TM; Jacob, CN; Ittycheria, CC; George, AM; Jacob, AG; Subramaniyam, S; Puthiyaveettil, J; Jayaprakash, R (March 2012). "Macrophage activation syndrome following Acinetobacter baumannii sepsis". International Journal of Infectious Diseases. 16 (3): e223–4. doi:10.1016/j.ijid.2011.12.002. PMID 22285540.
- ^ Sharma, A; Shariff, M; Thukral, SS; Shah, A (October 2005). "Chronic community-acquired Acinetobacter pneumonia that responded slowly to rifampicin in the anti-tuberculous regime". The Journal of Infection. 51 (3): e149–52. doi:10.1016/j.jinf.2004.12.003. PMID 16230195.
- ^ Jeong, HL; Yeom, JS; Park, JS; Seo, JH; Park, ES; Lim, JY; Park, CH; Woo, HO; Youn, HS (July–August 2011). "Acinetobacter baumannii isolation in cerebrospinal fluid in a febrile neonate". The Turkish Journal of Pediatrics. 53 (4): 445–7. PMID 21980849.
- ^ Hong, KB; Oh, HS; Song, JS; Lim, JH; Kang, DK; Son, IS; Park, JD; Kim, EC; Lee, HJ; Choi, EH (July 2012). "Investigation and control of an outbreak of imipenem-resistant Acinetobacter baumannii Infection in a Pediatric Intensive Care Unit". The Pediatric Infectious Disease Journal. 31 (7): 685–90. doi:10.1097/inf.0b013e318256f3e6. PMID 22466324. S2CID 1078450.
- ^ Lee, YK; Kim, JK; Oh, SE; Lee, J; Noh, JW (December 2009). "Successful antibiotic lock therapy in patients with refractory peritonitis". Clinical Nephrology. 72 (6): 488–91. doi:10.5414/cnp72488. PMID 19954727.
- ^ Lee, SY; Lee, JW; Jeong, DC; Chung, SY; Chung, DS; Kang, JH (August 2008). "Multidrug-resistant Acinetobacter meningitis in a 3-year-old boy treated with i.v. colistin". Pediatrics International. 50 (4): 584–5. doi:10.1111/j.1442-200x.2008.02677.x. PMID 18937759. S2CID 42715424.
- ^ Adams, D; Yee, L; Rimmer, JA; Williams, R; Martin, H; Ovington, C (February 2011). "Investigation and management of an A. baumannii outbreak in ICU". British Journal of Nursing. 20 (3): 140, 142, 144–7. doi:10.12968/bjon.2011.20.3.140. PMID 21378633.
- ^ Pencavel, TD; Singh-Ranger, G; Crinnion, JN (May 2006). "Conservative treatment of an early aortic graft infection due to Acinetobacter baumanii". Annals of Vascular Surgery. 20 (3): 415–7. doi:10.1007/s10016-006-9030-2. PMID 16602028. S2CID 38699601.
- ^ Gusten, WM; Hansen, EA; Cunha, BA (January–February 2002). "Acinetobacter baumannii pseudomeningitis". Heart & Lung. 31 (1): 76–8. doi:10.1067/mhl.2002.120258. PMID 11805753.
- ^ Fitzpatrick, MA; Esterly, JS; Postelnick, MJ; Sutton, SH (July–August 2012). "Successful treatment of extensively drug-resistant Acinetobacter baumannii peritoneal dialysis peritonitis with intraperitoneal polymyxin B and ampicillin-sulbactam". Annals of Pharmacotherapy. 46 (7–8): e17. doi:10.1345/aph.1r086. PMC 8454916. PMID 22811349. S2CID 20744216.
- ^ Patel, JA; Pacheco, SM; Postelnick, M; Sutton, S (15 August 2011). "Prolonged triple therapy for persistent multidrug-resistant Acinetobacter baumannii ventriculitis". American Journal of Health-System Pharmacy. 68 (16): 1527–31. doi:10.2146/ajhp100234. PMID 21817084.
- ^ Sullivan, DR; Shields, J; Netzer, G (June 2010). "Fatal case of multi-drug resistant Acinetobacter baumannii necrotizing fasciitis". The American Surgeon. 76 (6): 651–3. doi:10.1177/000313481007600636. PMID 20583528. S2CID 41059355.
