Gastritis
| Gastritis | |
|---|---|
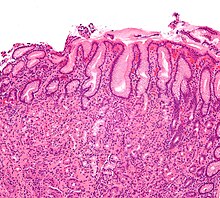 | |
| Micrograph showing gastritis. H&E stain. | |
| Specialty | Gastroenterology |
| Symptoms | Upper abdominal pain, nausea, vomiting, bloating, loss of appetite, heartburn[1][2] |
| Complications | Bleeding, stomach ulcers, stomach tumors, pernicious anemia[1][3] |
| Duration | Short or long term[1] |
| Causes | Helicobacter pylori, NSAIDs, alcohol, tobacco, cocaine, viruses, parasites, autoimmune[1] |
| Diagnostic method | Endoscopy, upper gastrointestinal series, blood tests, stool tests[1] |
| Differential diagnosis | Myocardial infarction, inflammation of the pancreas, gallbladder problems, peptic ulcer disease[2] |
| Treatment | Antacids, H2 blockers, proton pump inhibitors, antibiotics, sucralfate, bismuth subsalicylate,[1] antiemetics |
| Frequency | ~50% of people[4] |
| Deaths | 50,000 (2015)[5] |
Gastritis is the inflammation of the lining of the stomach.[1] It may occur as a short episode or may be of a long duration.[1] There may be no symptoms but, when symptoms are present, the most common is upper abdominal pain (see dyspepsia).[1] Other possible symptoms include nausea and vomiting, bloating, loss of appetite and heartburn.[1][2] Complications may include stomach bleeding, stomach ulcers, and stomach tumors.[1] When due to autoimmune problems, low red blood cells due to not enough vitamin B12 may occur, a condition known as pernicious anemia.[3]
Common causes include infection with Helicobacter pylori and use of nonsteroidal anti-inflammatory drugs (NSAIDs).[1] When caused by H. pylori this is now termed Helicobacter pylori induced gastritis, and included as a listed disease in ICD11.[6][7] Less common causes include alcohol, smoking, cocaine, severe illness, autoimmune problems, radiation therapy and Crohn's disease.[1][8] Endoscopy, a type of X-ray known as an upper gastrointestinal series, blood tests, and stool tests may help with diagnosis.[1] Other conditions with similar symptoms include inflammation of the pancreas, gallbladder problems, and peptic ulcer disease.[2]
Prevention is by avoiding things that cause the disease.[4][examples needed] Treatment includes medications such as antacids, H2 blockers, or proton pump inhibitors.[1] During an acute attack drinking viscous lidocaine may help.[9] If gastritis is due to NSAIDs these may be stopped.[1] If H. pylori is present it may be treated with a combination of antibiotics such as amoxicillin and clarithromycin.[1] For those with pernicious anemia, vitamin B12 supplements are recommended either by mouth or by injection.[3] People are usually advised to avoid foods that bother them.[10]
Gastritis is believed to affect about half of people worldwide.[4] In 2013 there were approximately 90 million new cases of the condition.[11] As people get older the disease becomes more common.[4] It, along with a similar condition in the first part of the intestines known as duodenitis, resulted in 50,000 deaths in 2015.[5] H. pylori was first discovered in 1981 by Barry Marshall and Robin Warren.[12]
Signs and symptoms
[edit]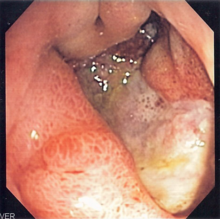
Many people with gastritis experience no symptoms at all. However, upper central abdominal pain is the most common symptom; the pain may be dull, vague, burning, aching, gnawing, sore, or sharp.[13] Pain is usually located in the upper central portion of the abdomen,[14] but it may occur anywhere from the upper left portion of the abdomen around to the back.
Other signs and symptoms may include the following:[13]
- Nausea
- Vomiting (may be clear, green or yellow, blood-streaked or completely bloody depending on the severity of the stomach inflammation)
- Belching (does not usually relieve stomach pain if present)
- Bloating
- Early satiety
- Loss of appetite
Causes
[edit]There are two categories of gastritis depending on the cause of the disease. There is erosive gastritis, for which the common causes are stress, alcohol, some drugs, such as aspirin and other nonsteroidal anti-inflammatory drugs (NSAIDs), and Crohn's disease. And, there is non-erosive gastritis, for which the most common cause is a Helicobacter pylori infection. [15][1]
Helicobacter pylori
[edit]Helicobacter pylori colonizes the stomachs of more than half of the world's population, and the infection continues to play a key role in the pathogenesis of a number of gastroduodenal diseases. Colonization of the gastric mucosa with Helicobacter pylori results in the development of chronic gastritis in infected individuals and, in a subset of patients, chronic gastritis progresses to complications (e.g., ulcer disease, stomach cancers, and some distinct extragastric disorders).[16] Gastritis caused by H. pylori infection is termed Helicobacter pylori induced gastritis, and listed as a disease in ICD11.[6][7] More than 80% of individuals infected with the bacterium are asymptomatic and it has been postulated that it may play an important role in the natural stomach ecology.[17]
Critical illness
[edit]Gastritis may also develop after major surgery or traumatic injury ("Cushing ulcer"), burns ("Curling ulcer"), or severe infections. Gastritis may also occur in those who have had weight loss surgery resulting in the banding or reconstruction of the digestive tract.[citation needed]
Diet
[edit]Evidence does not support a role for specific foods, including spicy foods and coffee, in the development of peptic ulcers.[18] People are usually advised to avoid foods that bother them.[10] There is little specific advice on diet published by authoritative sources. The National Health Service of the United Kingdom advises avoiding spicy, acidic or fried foods which may irritate the stomach.[19]
Pathophysiology
[edit]Acute
[edit]
Acute erosive gastritis typically involves discrete foci of surface necrosis due to damage to mucosal defenses.[20] NSAIDs inhibit cyclooxygenase-1, or COX-1, an enzyme responsible for the biosynthesis of eicosanoids in the stomach, which increases the possibility of peptic ulcers forming.[21][22][23] Also, NSAIDs, such as aspirin, reduce a substance that protects the stomach called prostaglandin. These drugs used in a short period are not typically dangerous. However, regular use can lead to gastritis.[24] Additionally, severe physiologic stress from sepsis, hypoxia, trauma, or surgery is also a common etiology for acute erosive gastritis, resulting in "stress ulcers". This form of gastritis can occur in more than 5% of hospitalized patients.[citation needed]
Also, alcohol consumption does not cause chronic gastritis. It does, however, erode the mucosal lining of the stomach; low doses of alcohol stimulate hydrochloric acid secretion. High doses of alcohol do not stimulate secretion of acid.[25]
Chronic
[edit]Chronic gastritis refers to a wide range of problems of the gastric issues.[20] The immune system makes proteins and antibodies that fight infections in the body to maintain a homeostatic condition. In some disorders the body targets the stomach as if it were a foreign protein or pathogen; it makes antibodies against, severely damages, and may even destroy the stomach or its lining.[24] In some cases bile, normally used to aid digestion in the small intestine, will enter through the pyloric valve of the stomach if it has been removed during surgery or does not work properly, also leading to gastritis. Gastritis may also be caused by other medical conditions, including HIV/AIDS, Crohn's disease, certain connective tissue disorders, and liver or kidney failure. Since 1992, chronic gastritis lesions are classified according to the Sydney system.[26]
Metaplasia
[edit]Mucous gland metaplasia, the reversible replacement of differentiated cells, occurs in the setting of severe damage of the gastric glands, which then waste away (atrophic gastritis) and are progressively replaced by mucous glands. Gastric ulcers may develop; it is unclear if they are the causes or the consequences. Intestinal metaplasia typically begins in response to chronic mucosal injury in the antrum and may extend to the body. Gastric mucosa cells change to resemble intestinal mucosa and may even assume absorptive characteristics. Intestinal metaplasia is classified histologically as complete or incomplete. With complete metaplasia, gastric mucosa is completely transformed into small-bowel mucosa, both histologically and functionally, with the ability to absorb nutrients and secrete peptides. In incomplete metaplasia, the epithelium assumes a histologic appearance closer to that of the large intestine and frequently exhibits dysplasia.[20]
Diagnosis
[edit]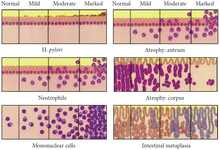
Often, a diagnosis can be made based on patients' description of their symptoms. Other methods which may be used to verify gastritis include:
- Blood tests:
- Blood cell count
- Presence of H. pylori
- Liver, kidney, gallbladder, or pancreas functions
- Urinalysis
- Stool sample, to look for blood in the stool
- X-rays
- Endoscopy, to check for stomach lining inflammation and mucous erosion
- Stomach biopsy, to test for gastritis and other conditions[27]
The OLGA staging frame of chronic gastritis on histopathology. Atrophy is scored as the percentage of atrophic glands and scored on a four-tiered scale. No atrophy (0%) = score 0; mild atrophy (1–30%) = score 1; moderate atrophy (31–60%) = score 2; severe atrophy (>60%) = score 3. These scores (0–3) are used in the OLGA staging assessment in each 10 compartment:[28]
| Corpus | |||||
|---|---|---|---|---|---|
| No atrophy (score 0) |
Mild atrophy (score 1) |
Moderate atrophy (score 2) |
Severe atrophy (score 3) | ||
| Antrum (including incisura angularis) | |||||
| No atrophy (score 0) | Stage 0 | Stage I | Stage II | Stage II | |
| Mild atrophy (score 1) | Stage I | Stage I | Stage II | Stage III | |
| Moderate atrophy (score 2) | Stage II | Stage II | Stage III | Stage IV | |
| Severe atrophy (score 3) | Stage III | Stage III | Stage IV | Stage IV | |
Treatment
[edit]Antacids are a common treatment for mild to medium gastritis.[29] When antacids do not provide enough relief, medications such as H2 blockers and proton-pump inhibitors that help reduce the amount of acid are often prescribed.[29][30]
Cytoprotective agents are designed to help protect the tissues that line the stomach and small intestine.[31] They include the medications sucralfate and misoprostol. If NSAIDs are being taken regularly, one of these medications to protect the stomach may also be taken. Another cytoprotective agent is bismuth subsalicylate.[32]
Several regimens are used to treat H. pylori infection. Most use a combination of two antibiotics and a proton pump inhibitor. Sometimes bismuth is added to the regimen.
History
[edit]In 1,000 A.D, Avicenna first gave the description of stomach cancer. In 1728, German physician Georg Ernst Stahl first coined the term "gastritis". Italian anatomical pathologist Giovanni Battista Morgagni further described the characteristics of gastric inflammation. He described the characteristics of erosive or ulcerative gastritis and erosive gastritis. Between 1808 and 1831, French physician François-Joseph-Victor Broussais gathered information from the autopsies of dead French soldiers. He described chronic gastritis as "Gastritide" and erroneously believed that gastritis was the cause of ascites, typhoid fever, and meningitis. In 1854, Charles Handfield Jones and Wilson Fox described the microscopic changes of stomach inner lining in gastritis which existed in diffuse and segmental forms. In 1855, Baron Carl von Rokitansky first described hypertrophic gastritis. In 1859, British physician, William Brinton first described about acute, subacute, and chronic gastritis. In 1870, Samuel Fenwick noted that pernicious anemia causes glandular atrophy in gastritis. German surgeon Georg Ernst Konjetzny noticed that both gastric ulcer and gastric cancer are the results of gastric inflammation. Shields Warren and Willam A. Meissner described the intestinal metaplasia of the stomach as a feature of chronic gastritis.[33]
See also
[edit]References
[edit]- ^ a b c d e f g h i j k l m n o p q r "Gastritis". The National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). November 27, 2013. Archived from the original on 6 March 2015. Retrieved 1 March 2015.
- ^ a b c d Rosen & Barkin's 5-Minute Emergency Medicine Consult (4 ed.). Lippincott Williams & Wilkins. 2012. p. 447. ISBN 978-1-4511-6097-0. Archived from the original on 2015-04-02.
- ^ a b c Varbanova M, Frauenschläger K, Malfertheiner P (Dec 2014). "Chronic gastritis - an update". Best Pract Res Clin Gastroenterol. 28 (6): 1031–42. doi:10.1016/j.bpg.2014.10.005. PMID 25439069.
- ^ a b c d Fred F. Ferri (2012). Ferri's Clinical Advisor 2013,5 Books in 1, Expert Consult - Online and Print,1: Ferri's Clinical Advisor 2013. Elsevier Health Sciences. p. 417. ISBN 978-0-323-08373-7. Archived from the original on 2016-03-05.
- ^ a b Wang H, Naghavi M, Allen C, Barber RM, Bhutta ZA, Carter A, et al. (8 October 2016). "Global, regional, and national life expectancy, all-cause mortality, and cause-specific mortality for 249 causes of death, 1980-2015: a systematic analysis for the Global Burden of Disease Study 2015". The Lancet. 388 (10053): 1459–1544. doi:10.1016/s0140-6736(16)31012-1. eISSN 1474-547X. ISSN 0140-6736. PMC 5388903. PMID 27733281. (GBD 2015 Mortality and Causes of Death Collaborators).
- ^ a b Malfertheiner P, Megraud F, Rokkas T, Gisbert JP, Liou JM, Schulz C, et al. (August 2022). "Management of Helicobacter pylori infection: the Maastricht VI/Florence consensus report" (PDF). Gut. 71 (9): 1724–1762. doi:10.1136/gutjnl-2022-327745. PMID 35944925.
- ^ a b "ICD-11 for Mortality and Morbidity Statistics". icd.who.int. Retrieved 9 January 2024.
- ^ Hauser, Stephen (2014). Mayo Clinic Gastroenterology and Hepatology Board Review. Oxford University Press. p. 49. ISBN 978-0-19-937333-8. Archived from the original on 2016-03-05.
- ^ Adams (2012). "32". Emergency Medicine: Clinical Essentials. Elsevier Health Sciences. ISBN 978-1-4557-3394-1. Archived from the original on 2016-08-15.
- ^ a b Webster-Gandy, Joan, Madden, Angela, Holdsworth, Michelle, eds. (2012). Oxford handbook of nutrition and dietetics (2nd ed.). Oxford: Oxford University Press, USA. p. 571. ISBN 978-0-19-958582-3. Archived from the original on 2017-09-08.
- ^ Vos T, Barber RM, Bell B, Bertozzi-Villa A, Biryukov S, Bolliger I, et al. (22 August 2015). "Global, regional, and national incidence, prevalence, and years lived with disability for 301 acute and chronic diseases and injuries in 188 countries, 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013". The Lancet. 386 (9995): 743–800. doi:10.1016/s0140-6736(15)60692-4. eISSN 1474-547X. ISSN 0140-6736. PMC 4561509. PMID 26063472. (Global Burden of Disease Study 2013 Collaborators).
- ^ Wang AY, Peura DA (October 2011). "The prevalence and incidence of Helicobacter pylori-associated peptic ulcer disease and upper gastrointestinal bleeding throughout the world". Gastrointestinal Endoscopy Clinics of North America. 21 (4): 613–635. doi:10.1016/j.giec.2011.07.011. ISSN 1558-1950. PMID 21944414.
- ^ a b "Gastritis Symptoms". eMedicineHealth. 2008. Archived from the original on 2008-12-06. Retrieved 2008-11-18.
- ^ "Gastritis". National Digestive Diseases Information Clearinghouse. National Institute of Diabetes and Digestive and Kidney Diseases. December 2004. Archived from the original on 2008-10-11. Retrieved 2008-10-06.
- ^ Vakil N (June 2021). "Gastritis - Digestive Disorders". MSD Manual Consumer Version. Merck & Co. Archived from the original on 13 August 2021. Retrieved 25 February 2022.
- ^ Kandulski A, Selgrad M, Malfertheiner P (1 August 2008). "Helicobacter pylori infection: a clinical overview". Digestive and Liver Disease. 40 (8): 619–626. doi:10.1016/j.dld.2008.02.026. PMID 18396114.
- ^ Blaser MJ (2006). "Who are we? Indigenous microbes and the ecology of human diseases" (PDF). EMBO Reports. 7 (10): 956–60. doi:10.1038/sj.embor.7400812. PMC 1618379. PMID 17016449. Archived (PDF) from the original on 2012-11-05.
- ^ Raphael Rubin, David S. Strayer, Emanuel Rubin, eds. (2012). Rubin's pathology : clinicopathologic foundations of medicine (Sixth ed.). Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins. p. 623. ISBN 978-1-60547-968-2. Archived from the original on 2015-04-02.
- ^ "Gastritis: Things you can do to ease gastritis". National Health Service. 2019-05-20. Retrieved 2021-08-29.
- ^ a b c Vakil N (January 2007). "Gastritis". Merck Manual - Professional Version. Merck & Co. Archived from the original on 25 January 2009. Retrieved 11 January 2009.
- ^ Dajani EZ, Islam K (1 August 2008). "Cardiovascular and gastrointestinal toxicity of selective cyclo-oxygenase-2 inhibitors in man" (PDF). Journal of Physiology and Pharmacology. 59 (Suppl 2): 117–133. ISSN 1899-1505. OCLC 165902827. PMID 18812633.[permanent dead link]
- ^ Yokoyama C, Tanabe T (15 December 1989). "Cloning of human gene encoding prostaglandin endoperoxide synthase and primary structure of the enzyme". Biochemical and Biophysical Research Communications. 165 (2): 888–94. doi:10.1016/S0006-291X(89)80049-X. eISSN 1090-2104. ISSN 0006-291X. LCCN 61065129. OCLC 1532958. PMID 2512924.
- ^ Funk CD, Funk LB, Kennedy ME, Pong AS, Fitzgerald GA (1 June 1991). "Human platelet/erythroleukemia cell prostaglandin G/H synthase: cDNA cloning, expression, and gene chromosomal assignment". The FASEB Journal. 5 (9): 2304–2312. doi:10.1096/fasebj.5.9.1907252. eISSN 1530-6860. ISSN 0892-6638. LCCN 87644294. OCLC 1096896944. PMID 1907252. S2CID 46147389.
- ^ a b Siegelbaum J (23 August 2019). "GI Health Resources > Gastritis". Jackson Siegelbaum Gastroenterology. Archived from the original on 15 June 2021. Retrieved 25 February 2022.
- ^ Wolff G (1989). "[Effect of alcohol on the stomach]" [Effect of alcohol on the stomach]. Gastroenterologisches Journal (in German). 49 (2): 45–49. ISSN 0863-1743. PMID 2679657. S2CID 23245888.
- ^ Mayo Clinic Staff (April 13, 2007). "Gastritis". MayoClinic. Archived from the original on December 8, 2008. Retrieved 2008-11-18.
- ^ "Exams and Tests". eMedicinHealth. 2008. Archived from the original on 2008-12-11. Retrieved 2008-11-18.
- ^ Carrasco G, Corvalan AH (2013). "Helicobacter pylori-Induced Chronic Gastritis and Assessing Risks for Gastric Cancer". Gastroenterol Res Pract. 2013: 393015. doi:10.1155/2013/393015. PMC 3745848. PMID 23983680.
 This article incorporates text available under the CC BY 3.0 license.
This article incorporates text available under the CC BY 3.0 license.
- ^ a b Zajac P, Holbrook A, Super ME, Vogt M (March–April 2013). "An overview: Current clinical guidelines for the evaluation, diagnosis, treatment, and management of dyspepsia". Osteopathic Family Physician. 5 (2): 79–85. doi:10.1016/j.osfp.2012.10.005.
- ^ Boparai V, Rajagopalan J, Triadafilopoulos G (2008). "Guide to the use of proton pump inhibitors in adult patients". Drugs. 68 (7): 925–47. doi:10.2165/00003495-200868070-00004. PMID 18457460. S2CID 29732662.
- ^ Fashner J, Gitu AC (15 February 2015). "Diagnosis and Treatment of Peptic Ulcer Disease and H. pylori Infection". American Family Physician. 91 (4): 236–42. PMID 25955624.
- ^ "Gastritis". The Lecturio Medical Concept Library. Retrieved 22 July 2021.
- ^ Gyula M (16 January 2013). "Chapter 1: Diagnosis of Gastritis – Review from Early Pathological Evaluation to Present Day Management" (PDF). Current Topics in gastritis. University of Pécs. pp. 1–19. ISBN 978-953-51-0907-5. Retrieved 10 July 2018.
Further reading
[edit]- Vakil N (June 2021). "Gastritis - Digestive Disorders". MSD Manual Consumer Version. Merck & Co. Archived from the original on 13 August 2021. Retrieved 25 February 2022.
